Families For Life | Genetic Disorder: Is My Baby at Risk?
Genetic testing is voluntary. Clues can be gained from keeping family history health records.
You may be concerned if you have a family history of babies who were born abnormal, or you are worried you might have an unknown genetic problem which may be passed on to your offsprings.
Many clues can be gained from keeping family history health records. A genetic counsellor may be able to advise you accordingly.
What causes genetic disorders?
Every child inherits 23 pairs of chromosomes from each parent -- one from the mum and one from the dad. Each chromosome contains thousands of genes.
Genetic disorders can be caused by abnormalities in the number of chromosomes (which are your genetic makeup) or a defect in a single gene.
In most instances, the genetic disorders are caused by a single gene defect -- or what is commonly known as Mendelian genetics.
These gene defects may be classified as:
Dominant -- one of the genes is defective and overrides the normal gene, thus the presence of one abnormal gene within the gene pair is adequate for the manifestation of the disease (e.g. polycystic kidney disease, achondroplasia or dwarfism).
Recessive -- contrary to the above, the manifestation of the disease requires both genes in the gene pair to be defective (e.g. albinism, cystic fibrosis or [thalassemia].
Sex-linked (X-linked) -- the defective gene is present in the X chromosome and can be either recessive or dominant. Hence X-linked recessive gene defects tend to manifest in males where the gene is of a XY genotype while X-linked dominant gene defects can manifest in both males (XY) or females (XX) (e.g. hemophilia, muscular dystrophy).
Carriers of recessive defective genes may not have any manifestation and may be unaware. However, if both parents are carriers of the same abnormal gene, there is a 25% chance of having an affected baby for each pregnancy.
Carrier testing can be done to determine if you carry one of the two abnormal genes that can cause a specific recessive disorder. Unfortunately, it is not yet possible to test for all genetic conditions.
What is my risk of genetic disease?
In most instances, we are all at a low risk for inherited genetic diseases. However, this risk may increase under certain circumstances. These include a significant family history, ethnicity and heritage.
Some genetic syndromes are more common in certain ethnic groups. For instance, 1 in 25 Caucasians of European descent carry the cystic fibrosis mutation gene. Sickle cell trait is more common in Blacks and thalassaemia (an inherited form of anemia) is prevalent in those of Mediterranean or Asian descent.
Do I need to see a genetic counsellor?
If you are in any of the following groups, your obstetrician may refer you to see a genetic counsellor:
You had given birth to a genetically abnormal child in your previous pregnancy.
You have had recurrent pregnancy losses (3 or more consecutive miscarriages).
You or your partner have blood tests which showed both of you are carriers of a genetic disorder.
You have a known family history of a serious heritable disorder.
You have a positive screening test for foetal defect.
How do genetic tests work?
As these tests carry some risk in the pregnancy, genetic testing will only be conducted if there is a significant chance of the disease manifesting in the baby.
A genetic test involves examining a DNA sample from a patient. The DNA sample can come from any human tissue, most commonly from blood samples.
Prenatal diagnostic testing is offered after prenatal screening tests suggest a higher possibility of a genetic disorder, or as a first line diagnostic testing in couples where a specific genetic disorder is present. Prenatal genetic diagnosis provides couples with the option of terminating an affected pregnancy, planning foetal treatment or preparing for the birth of an abnormal child.
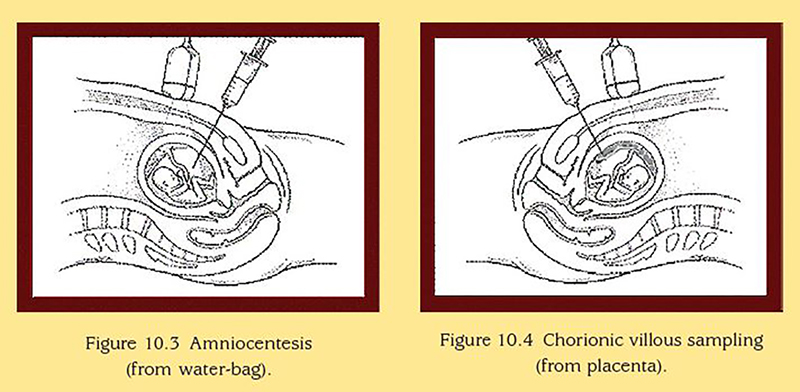
In general, the test requires a specimen from the foetus, placenta or amniotic fluid for various specific genetic diseases.
Other techniques of prenatal genetic diagnosis include radiological studies like MRI, detailed ultrasound of the foetus, and pre-implantation genetic diagnosis in which early embryos created by in-vitro fertilization (test-tube babies) are evaluated to determine the presence of genetic conditions.
Unaffected embryos are then selected for implantation into the womb.
Once the sample is obtained, there are several methods of analysis, depending on the type of disorder. For example, chromosomal abnormalities are evaluated by cytogenetic analysis; single gene disorders and inborn errors of metabolism by DNA analysis.
There are many conditions which are amenable to testing in:
DNA laboratory (thalassaemia, spinal muscular atrophy, fragile X syndrome and myotonic dystrophy)
paediatric laboratory (Duchenne Muscular Dystrophy, Hemophilia A)
overseas centres (cystic fibrosis)
Let your genetic counsellor or obstetrician advise you accordingly.
What are some of the issues relating to genetic testing?
It is important to understand that genetic testing is purely voluntary and you should not feel coerced into doing it.
The aim of genetic testing is to allow you to predict if you will deliver a normal baby. A negative testing gives you reassurance and a positive result allows you to make informed and deliberate choices with regards to pregnancy continuation or termination (abortion).
There are potential risks of genetic testing. This includes psychological distress as the individual faces the prospect of possibly having a hereditary condition and the difficult decision of whether to undergo genetic testing to confirm.
Genetic testing may also affect other family members as they may share different views on testing.
A positive gene test result may also cause potential genetic discrimination by employers and insurers.
By Dr TAN Thiam Chye, Dr TAN Kim Teng, Dr TAN Heng Hao, Dr TEE Chee Seng John,
KK Women's and Children's Hospital
Sources:
The New Art and Science of Pregnancy and Childbirth, World Scientific 2008.
Copyright © 2016 HealthHub.sg. All rights reserved.