Families For Life | Eczema-Young Children
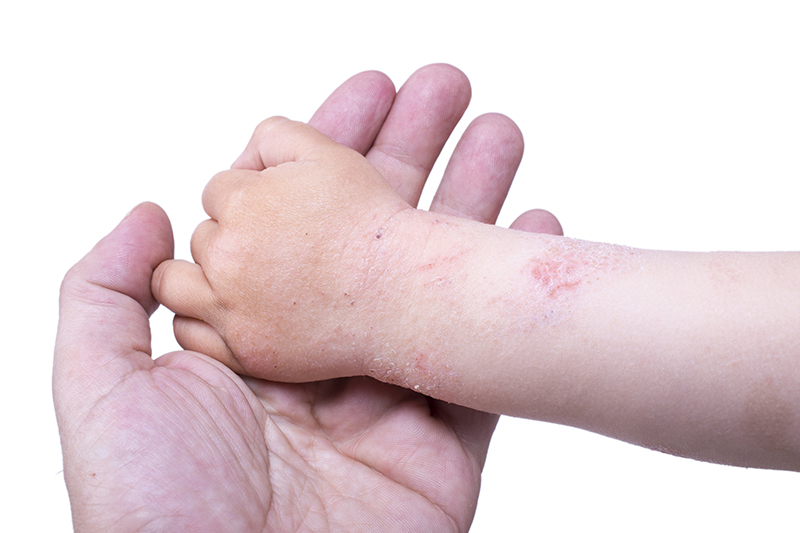
Eczema is a common skin condition that happens in about one in five babies. Children with eczema have dry, sensitive skin. They also get itchy, red, scaly patches on their skin. If you think your child might have eczema, you should see your General Practitioner (GP). Eczema is also called dermatitis.
Causes of eczema
Eczema has a genetic basis – this means it tends to run in families. Children with eczema often have other allergy-type conditions like asthma or hayfever.
Eczema might flare up:
after contact with irritating chemicals like soaps or bubble baths, or irritating fabrics like woollen underlays or polyester garments
after viral or bacterial infections
after exposure to substances like dust mite or animal fur
after exposure to foods that your child is allergic to
when your child gets too hot
when your child is stressed.
Often there’s no obvious cause for a flare-up.
In a few children, diet can make eczema worse, although it’s often hard to say which food is causing the problem.
Eczema is not contagious.
Eczema symptoms
Children with eczema have very itchy, scaly, red patches of skin, usually on their cheeks, in their elbow creases and behind their knees. It might also appear on children’s necks, bodies, hands and feet. Eczema locations change with time. For example, when children start to crawl you might see eczema coming up on the exposed skin of their lower legs.
Eczema can weep, develop cracks and even bleed, especially if your child scratches a lot because of the itch. Bacterial infections like Staphylococcus and viral infections like herpes can get into the skin through these cracks. This leads to light-brown crusts, blisters and/or pain.
Eczema usually comes and goes. In between flare-ups, the skin might look thickened and dry (this is called ‘lichenification’). But in mild eczema the skin goes back to normal with no scarring.
Eczema usually starts in the first few months of life. At first, you might see it only on your child’s face and scalp, or in the diaper region. Most children tend to ‘grow out’ of eczema by adolescence, but some people have eczema throughout their adult lives.
When to see your doctor about eczema
You should take your child to see your GP if:
you think your child might have eczema for the first time
your child’s eczema is weeping or bleeding
you’ve been treating your child’s eczema as usual, but there’s no significant improvement after a few days
your child is having trouble sleeping because the rash is so itchy
your child is generally unwell, in addition to the rash
the eczema is painful or has developed pus
you’re not sure that the rash actually is eczema.
Treatment for eczema
Eczema is chronic and can’t be cured, but it can be managed. The key to preventing eczema flare-ups is to treat symptoms as soon as they appear.
Eczema gets worse when skin is dry. Applying oils and moisturising creams directly to your child’s skin helps to stop the skin from drying out. Your child should use them every day, even when there’s no eczema.
If your young child is scratching at his rash, try putting cotton mittens on his hands at night. Cut his nails short, and keep them clean. If he’s scratching really hard, see your pharmacist or doctor to discuss using an antihistamine medication for a few days. This might give your child some rest, and help the flare-up to settle.
Another way to soothe the itch is to put a ‘wet dressing’ on the eczema. Start by applying a generous smear of a greasy moisturising ointment over the eczema. Wet a soft towel with cool tap water and put it on the eczema. Leave the towel for 15-30 minutes. Remove the towel and apply another smear of moisturiser if the first lot has been absorbed.
When you bathe your child, keep the baths short. Use warm but not hot water. Bathe your child no more than once a day. Add a moisturising bath oil to the bath. You can buy these oils without a prescription. Avoid fragranced or ‘fancy’ bath additives. For babies and toddlers, you could wash your child’s face and bottom rather than giving your baby a full bath.
Don’t use soap on young children. They don’t need it, it dries out the skin, and it can make the eczema worse. Older children can use a mild soap substitute under the armpits and around the genitals. They can also use a moisturising cream like sorbolene or a cream containing paraffin during and after washing – this will help stop the skin from drying out.
Cortisone ointments and creams are the main eczema treatments. You should apply these ointments several times a day to affected areas, or according to your doctor’s instructions. For mild eczema, you can buy mild corticosteroids over the counter at pharmacies. For more serious eczema, your child will need to see a doctor to get a prescription for a stronger corticosteroid.
Other eczema treatments include pimecrolimus, a non-steroidal cream. Doctors might prescribe this cream for children with mild to moderate eczema on the face and body folds.
If your child uses any of these moisturisers and prescription ointments, take them with you when you’re out. Put them on your child as soon as she starts to scratch. You can also ask anyone who cares for your child to put the treatments on your child if you’re not around.
If your child’s eczema rash gets infected, your doctor will prescribe an antibiotic cream or a course of oral antibiotics.
If your child’s eczema doesn’t improve despite all these measures, you might want to talk with your doctor about taking your child to see a dermatologist.
Prevention of eczema
The main way to prevent eczema in your child is to avoid things that irritate your child’s skin:
Dress your child in cotton underwear and clothes.
Keep your child cool, because overheating makes the itch worse, as do hot baths or showers.
Avoid the use of soaps and bath preparations.
Give your child short baths or showers because water can dry out your child’s skin. Bathe your child no more than once a day.
Your child can swim in chlorinated water, but you should apply moisturiser all over before swimming. After swimming, wash the skin in a cool shower or bath, and apply more moisturiser. Salt water might improve eczema.
If you think your child’s eczema is caused by a food allergy, but you can’t work out which food is the problem, you could talk with your doctor about allergy testing.
© raisingchildren.net.au, translated and adapted with permission